By Cesilia Nishi, BSc(Pharm) ACPR PharmD
Coronavirus disease 2019 (COVID-19), the disease caused by the virus SARS-CoV-2, maintains a strong grip on the world with over 92 million cases and 2 million deaths attributed to the disease worldwide to date1.
Since the start of the pandemic, there has been a fervent search for pharmacologic therapeutics, from antivirals to therapies to treat this infection and modulate the immune response to the virus. From the outset, international bodies such as the World Health Organization (WHO) have recommended against the use of investigational therapies for COVID-19 outside of clinical trials. As such, a need to provide consistent and evidence-based therapeutic recommendations was quickly identified and the British Columbia COVID-19 Therapeutics Committee (CTC) was formed in March 20202.
Initially, the committee consisted of frontline clinicians, including pharmacists, from Vancouver General Hospital and St. Paul’s Hospital, but has quickly expanded to have representation from all health authorities in the province, the Pharmaceutical Services Division of the Ministry of Health, as well as researchers. Our clinician committee members represent a wide variety of specialties including: anesthesia, antimicrobial stewardship, critical care, emergency medicine, family medicine, immunology, infectious diseases, internal medicine, hematology, medical microbiology, pediatrics, rheumatology, and pharmacy. Of our 43 committee members, 11 are pharmacists.
The CTC holds weekly to biweekly virtual meetings to review the latest literature on various COVID-19 therapeutics and provide recommendations on the use of these agents. These recommendations are updated regularly on the British Columbia Centre for Disease Control (BCCDC)’s website3. A small group of members have been assigned specific therapeutics to ensure that recommendations reflect the latest available published, as well as non-peer reviewed, unpublished, literature. The most recent version of the recommendations can be found at: bccdc.ca/health-professionals/clinical-resources/covid-19-care/clinical-care/treatments.
Therapies that have been investigated for use in COVID-19 can be divided in the following subcategories: antivirals, immune modulators, and supportive therapies. Notable antivirals and immune modulating therapies will be discussed below.
Antivirals:
Despite initial excitement surrounding benefits seen with antivirals in small observational studies or case series, the results of the majority of published randomized controlled trials for antivirals have been negative to date.
Lopinavir/ritonavir:
Lopinavir/ritonavir (Kaletra®), a protease inhibitor combination used in the management of human immunodeficiency virus (HIV), gained interest in its use for COVID-19 based on its in vitro activity against other coronaviruses such as Sever Acute Respiratory Syndrome (SARS) and Middle East Respiratory Syndrome (MERS). Cao et al5. conducted an open label, randomized controlled trial of lopinavir/ritonavir 400/100 mg orally twice daily for 14 days plus standard care versus standard care alone in 199 adult patients hospitalized with COVID-19 pneumonia requiring supplemental oxygen in Wuhan, China. For their primary outcome of time to clinical improvement, lopinavir/ritonavir did not improve the time to clinical improvement. However, due to the availability of remdesivir in China, this study was suspended early and was deemed to be underpowered to detect a difference. Subsequently, the RECOVERY Collaborative group—a clinical trial of possible treatments for people in the U.K. admitted to hospital with severe COVID-19 infection—has reported that lopinavir/ritonavir did not reduce 28-day mortality, duration of hospital stay, risk of progression to invasive mechanical ventilation or death6. The WHO’s international Solidarity Trial Consortium, which has enrolled nearly 12,000 patients in 500 hospitals in over 30 countries, has recently published similar findings in their interim analysis7.
Hydroxychloroquine/chloroquine:
The use of hydroxychloroquine and chloroquine for COVID-19 quickly gained notoriety following the publication of the non-randomized study by Gautret et al., which suggested rapid viral clearance with hydroxychloroquine particularly when used in combination with azithromycin8. However, due to several methodological issues with this study, the CTC recommended use only within randomized controlled trials. Since then, the RECOVERY Collaborative group and the Solidarity Trial Consortium have published the hydroxychloroquine portion of their studies, both of which have not found benefit in mortality7,9. The RECOVERY Collaborative group also found that patients who received hydroxychloroquine had a longer duration of hospitalization and lower probability of survival, and also reported a numerically higher rate of cardiac death compared to the control group.
Remdesivir:
Remdesivir is a monophosphoramidate prodrug of an adenosine analogue that has broad activity against several viruses including coronaviruses. The first published randomized controlled trial of remdesivir in COVID-19, conducted by Wang Y et al.10, compared 10 days of remdesivir therapy versus placebo in adults hospitalized with COVID-19 pneumonia in Wuhan, China. Due to control of COVID-19 in Wuhan, this trial enrolled only 236 patients compared to the planned 453 patients. For the primary outcome of time to clinical improvement, no statistically significant difference between the groups was found. Of note, 65% and 68% of patients received corticosteroid treatment, respectively, in the two arms of this trial.
The ACTT-1 trial, a National Institute of Health-sponsored, randomized, controlled study, evaluated 10 days of remdesivir versus placebo in adults hospitalized with COVID-19 pneumonia11. For the primary outcome of time to clinical recovery, remdesivir was associated with a shorter time to recovery than placebo (10 days versus 15 days). This was statistically significant for patients that required supplemental oxygen but not mechanical ventilation or high flow oxygen at baseline. No difference in mortality was observed. Overall, only 23% of patients received corticosteroids. Based on the ACTT-1 trial, organizations such as the Infectious Diseases Society of America have recommended the use of remdesivir for hospitalized patients with severe COVID-1912.
In contrast, the WHO has issued a conditional recommendation against the use of remdesivir in hospitalized patients based on publication of the interim results of the remdesivir portion of the Solidarity Trial Consortium study7. In the interim analysis of their open-label study, remdesivir was not associated with reduction in mortality, nor did it reduce initiation of ventilation or duration of hospital stay.
As the ACTT-1 study had relatively low use of corticosteroid (see corticosteroid section below), it is uncertain the extent of benefit remdesivir will have currently in hospitalized patients with COVID-19 where corticosteroids are now a standard of care. Thus, the CTC currently continues to recommend the use of remdesivir in the context of randomized controlled trials.
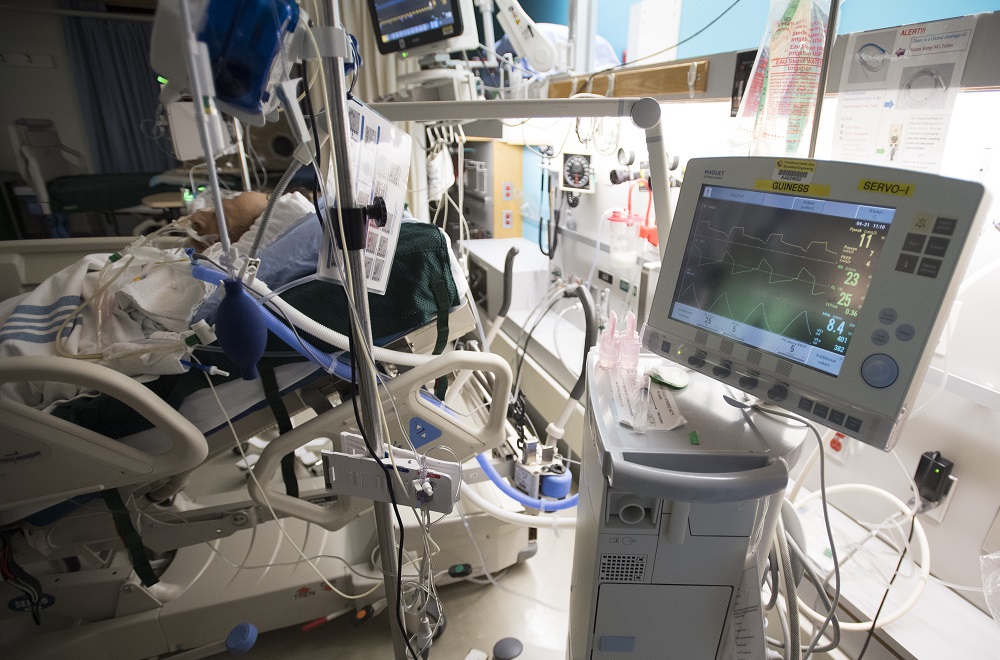
A patient is attached to a ventilator in the COVID-19 intensive care unit at St. Paul’s Hospital in Vancouver. (Jonathan Hayward/Canadian Press)
Immune Modulators:
Corticosteroids:
Initially, corticosteroids were not recommended for use in COVID-19 due to evidence of harm observed in other coronavirus infections, such as Severe Acute Respiratory Syndrome (SARS), and concern of delayed viral clearance4. However, with the publication of the corticosteroid portion of the RECOVERY trial13, corticosteroids are now considered standard of care for any hospitalized patient with COVID-19. In the dexamethasone portion of this large open-label study, hospitalized patients with COVID-19 were randomized to receive dexamethasone 6 mg orally or intravenously daily for up to 10 days versus standard of care. Dexamethasone was associated with a statistically significant reduction in 28-day mortality compared to standard of care.
Tocilizumab
Tocilizumab, a monoclonal antibody specific for interleukin-6, used for rheumatologic conditions such as rheumatoid arthritis and giant cell arteritis, gained interest in its use for the treatment of patients who develop severe hypoxemic respiratory failure. In such patients, elevations in interleukin-6, ferritin, and C reactive protein levels may be observed, similar to patients with cytokine storm following chimeric antigen receptor (CAR) T cell therapy, for which tocilizumab has been used14. Initial results from clinical trials have been mixed. The BACC Bay Tocilizumab Trial Investigators found that tocilizumab, as compared to placebo, was not effective in preventing need for intubation or death in moderately-ill patients admitted to hospital with COVID-1915. The COVACTA trial, which compared tocilizumab to placebo in patients admitted to hospital with COVID-19, did not find a difference in clinical status at day 2816. EMPACTA found that tocilizumab reduced the likelihood of mechanical ventilation or death at day 28 in patients hospitalized with COVID-19, but not receiving mechanical ventilation17. This study did not find a survival benefit with tocilizumab therapy.
More recently, the pre-print of the preliminary report of the interleukin-6 receptor antagonist portion of the open label REMAP-CAP trial was released18. Adults hospitalized with COVID-19 within 24 hours of receiving cardiovascular and/or respiratory organ support, were randomized to receive tocilizumab, 8 mg/kg (to a maximum of 800 mg) intravenously (with an optional second dose given 12-24 hours after the first dose)(n=353), sarilumab 400 mg intravenously (n=48), or control (standard care)(n=402). For the primary outcome of organ support free days up to day 21, tocilizumab was associated with an odds ratio of 1.64 (95% credible interval 1.25, 2.14) as compared to control. Odds ratio of hospital survival with tocilizumab was 1.64 (95% credible interval 1.14, 2.35). Statistically significant benefit was also found with sarilumab. Nine versus 11 serious adverse events were reported in the tocilizumab and control groups, respectively. Based on the release of this preliminary report, the CTC currently recommends a single dose of tocilizumab in critically ill patients with COVID-19 within 24 hours of respiratory or cardiovascular support.
What can community pharmacists expect to see for patients with COVID-19 recently discharged from hospital?
All of the therapies discussed in this article were studied for use during hospitalization only. However, hospitalization, particularly with COVID-19, is associated with a number of complications that may require ongoing pharmacologic treatment. Like with any other hospitalization, nosocomial infections such as urinary tract infections, hospital acquired pneumonias and Clostridium difficile-associated diarrhea may occur. Thus, patients may be discharged with prescriptions to complete their anti-infective therapy. While dexamethasone therapy specifically for the treatment of COVID-19 was studied for use in hospital only, various complications in hospital such as acute respiratory distress syndrome, may require higher doses of corticosteroid, resulting in patients being discharged home with tapering doses of corticosteroid. Finally, coagulopathies are common with COVID-19, resulting in thromboembolism4, therefore some patients may require ongoing anticoagulation on hospital discharge.
The landscape for the management of COVID-19 is rapidly changing and it is important as health-care professionals to stay abreast of these changes. For further details on the therapies discussed in this article as well as many other therapies not included, please refer to the BCCDC COVID-19 Treatment page.
Cesilia Nishi is a Infectious Diseases clinical pharmacy specialist at Vancouver General Hospital. She is also a clinical assistant professor at the UBC Faculty of Pharmaceutical Sciences, and an associate member of the Division of Infectious Diseases with the UBC Faculty of Medicine.
References
- World Health Organization. WHO Coronavirus Disease (COVID-19) Dashboard. Accessed December 19, 2020: www.Covid19.who.int
- British Columbia COVID-19 Therapeutics Committee. COVID-19 pharmacologic therapy guidance for BC. Brit Col Med J 2020; 62(5):161-2.
- British Columbia COVID-19 Therapeutics Committee. BC Centre for Disease Control. Clinical reference group recommendations: therapies for COVID-19. Updated December 1, 2020. Accessed December 19, 2020: http://www.bccdc.ca/health-professionals/clinical-resources/covid-19-care/clinical-care/treatments
- World Health Organization. Clinical management of COVID-19: interim guidance. May 27, 2020. Accessed December 19, 2020: https://www.who.int/publications/i/item/clinical-management-of-covid-19
- Cao B, Wang Y, Wen D et al. A trial of lopinavir-ritonavir in adults hospitalized with severe Covid-19. N Engl J Med 2020;382:1787-99.
- The RECOVERY Collaborative Group. Lopinavir-ritonavir in patients admitted to hospital with COVID-19 (RECOVERY): a randomised, controlled, open-label platform trial. Lancet 2020; 396:1345-52.
- WHO Solidarity Trial Consortium. Repurposed antiviral drugs for Covid-19 – interim WHO Solidarity Trial results. N Engl J Med 2020;
- Gautret P, Lagier JC, Parola P et al. Hydroxychloroquine and azithromycin as a treatment of COVID-19: results of an open-label non-randomized clinical trial. Int J Antimicrob Agent 2020;56(1):
- The RECOVERY Collaborative Group. Effect of hydroxychloroquine in hospitalized patients with Covid-19. N Engl J Med 2020; 383:2030-40.
- Wang Y, Zhang D, Du G et al. Remdesivir in adults with severe COVID-19; a randomised, double-blind, placebo-controlled, multicentre trial. Lancet 2020;395:1569-78.
- Beigel JH, Tomashek KM, Dodd LE et al. Remdesivir for the treatment of Covid-19 – final report. N Engl J Med 2020;383:1813-26.
- Bhimraj A, Morgan RL, Shumaker AH et al. Infectious Diseases Society of America guidelines on the treatment and management of patients with COVID-19. Updated December 2, 2020. Accessed December 19, 2020: https://www.idsociety.org/globalassets/idsa/practice-guidelines/covid-19/treatment/idsa-covid-19-gl-tx-and-mgmt-v3.5.1.pdf
- The RECOVERY Collaborative Group. Dexamethasone in hospitalized patients with Covid-19 – preliminary report. N Engl J Med 2020. DOI: 10.1056/NEJMoa2021436.
- Fajgenbaum DC, June CH. Cytokine storm. N Engl J Med 2020; 383:2255-73.
- Stone JH, Frigault MJ, Serling-Boyd NJ, et al. Efficacy of tocilizumab in patients hospitalized with Covid-19. N Engl J Med 2020; 383:2333-44.
- Rosas I, Braü N, Waters M et al. Tocilizumab in hospitalized patients with COVID-19 pneumonia. September 12, 2020. Accessed from: https://www.medrxiv.org/content/10.1101/2020.08.27.20183442v2. Preprint.
- Salama C, Han J, Yau L et al. Tocilizumab in patients hospitalized with Covid-19 pneumonia. N Engl J Med 2021;384:20-30.
- Gordon AC, Mouncey PR, Al-Beidh F et al. Interleukin-6 receptor antagonists in critically ill patients with Covid-19 – preliminary report. January 9, 2021. Accessed from: https://www.medrxiv.org/content/10.1101/2021.01.07.21249390v2.full-text Preprint.
